Applying “Well After Service”: the Veteran Wellness Model
As of November 1, 2020, National Veterans Intermediary (NVI) is called the Local Partner Network. Older content may reference our original name.
In April 2012, the Center for a New American Security (CNAS) published a report entitled “Well After Service: Veteran Reintegration and American Communities.” The publication, co-authored by NVI’s President, Nancy Berglass, and Dr. Margaret Harrell (now Director of BWF’s Charitable Investments program), shares findings and recommendations that remain relevant today–and highlights systemic issues that are not yet resolved. In this blog series, we will explore some key takeaways from “Well After Service,” and how collaboratives can apply this information in their work.
Defining Veteran Wellness
In “Well After Service”, Berglass and Harrell provide a thoughtfully researched definition of veteran wellness. Before exploring the four dimensions of wellness, it’s worth understanding the definition that informs the Veteran Wellness Model, and how the authors created it. Beginning with a survey of traditional definitions from influential civilian and military organizations, the authors applied each to the the unique attributes and circumstances of both military life and the veteran’s experience as a civilian, and crafted a new definition that is comprehensive and functional, in direct relation to evidence about how veterans live their lives:
“Physical Well-Being and Psychological Well-Being are the satisfactory and sufficient conditions permitting individuals to function as necessary. Physical and psychological well-being are each informed by four dimensions: social/personal relationships, health, fulfillment of material needs and purpose. These dimensions are interrelated and mutually supporting. When an individual achieves both physical and psychological well-being, that individual experiences basic wellness.
Veteran Wellness is the dynamic and multidimensional quality of one’s existence overall, as informed by both civilian and military experiences and circumstances. It reflects both physical and psychological well-being and is thus based on the four interrelated dimensions listed above. One strives toward increased wellness.”
Mapping Resources
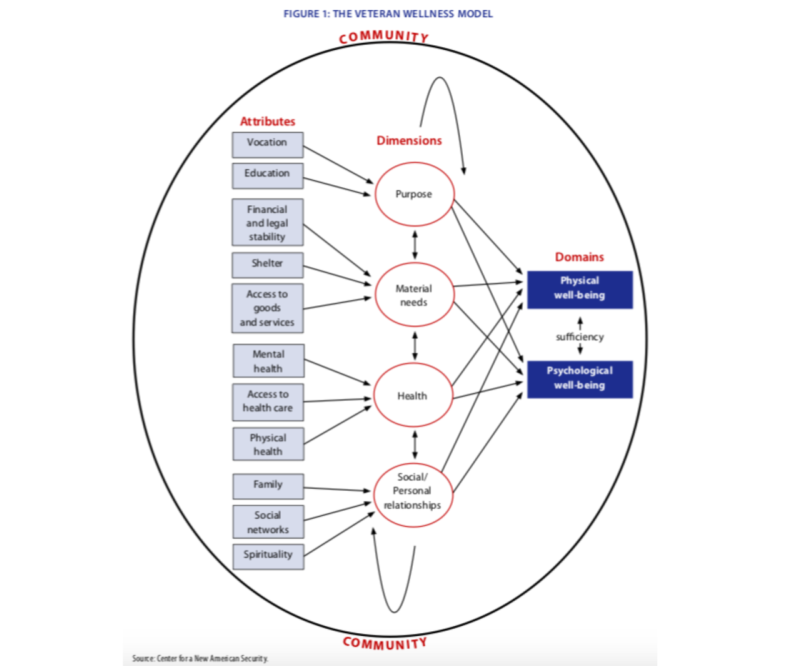
The four dimensions and respective attributes that contribute to physical and psychological well-being are defined in this chart depicting the Veteran Wellness Model:
The attributes, as well as the dimensions they inform, offer a helpful framework for resource mapping. Try using the Veteran Wellness Model to frame an iteration of your collaborative’s resource mapping efforts. The dimensions and attributes are laid out below; the bulleted questions may be treated as prompts as you work through the model.
Purpose
Vocation
- What is the employment outlook in your area?
- What organizations and individuals–public, private, and independent sector–are in a position to support veteran employment outcomes? Which are currently committed to veteran employment?
- Are there opportunities for veterans who are not seeking paid work to use their skills (volunteering, pro-bono work, board opportunities)?
Education
- Are diverse educational opportunities available in your area?
- Are your university systems equipped to serve nontraditional students?
- For student veterans, are there opportunities for non-GI Bill income during breaks that also promote career exploration?
- Are training, OJT, and apprenticeship opportunities well-developed?
Material Needs
Financial and legal stability
- Evaluate wage and cost of living information in your service area–are they balanced?
- Are unemployment insurance, supplemental nutrition programs, and other assistance programs easy to access?
Shelter
- How is the housing market in your area (property and rental)?
- Are there emergency shelters? Grant per diem or transitional housing programs? What eligibility gaps exist?
Access to goods and services
- Considering taxes, registration, inspection, and climate, and road conditions, how expensive is it to own and maintain a vehicle?
- How does public transportation serve your area? Is scheduling and routing sufficient to support access to necessities, goods, and services? How about employment?
Health
Mental Health
- Is mental health treatment accessible?
- How long does it take to get seen?
- Who may be missing out on services due to eligibility criteria, access, or availability?
Access to health care
- Is regular health care available? Preventative care? Specialty care?
- Can veterans access health care in their own communities?
- Is telehealth available to rural or housebound veterans?
Physical health
- What options are available for movement/fitness practices? Considering costs of equipment and membership, are they affordable?
- Are there adaptive sports and recreation opportunities?
- Is nutritious food available to veterans of all income levels?
Social/Personal relationships
Family
- Do services provide wrap-around care inclusive of veteran families?
- Is relationship and family counseling available?
Social networks
- Are veterans service organization chapters in your area inclusive?
- Are there opportunities for socialization or interest-based groups that are recovery-friendly?
Spirituality
- Do faith-based organizations play a role in your collaborative’s efforts?
After considering these questions, note the areas of strength and need that were highlighted through your exploration of the Veterans Wellness Model. Lastly, which stakeholders might your collaborative convene around your community’s areas of need?









